There's underlying urgency in her voice as an emergency dispatcher rolls half a dozen vehicles toward twisted metal and broken bodies, an intersection where spinning tires still claw at the nighttime chill.
In newsrooms across Lincoln, reporters stop tapping on keyboards to catch more details. Police in squad cars flick on sirens. New wheels begin to spin faster.
Updates come encoded in medical lingo: agonal breathing, additional EMS requested.
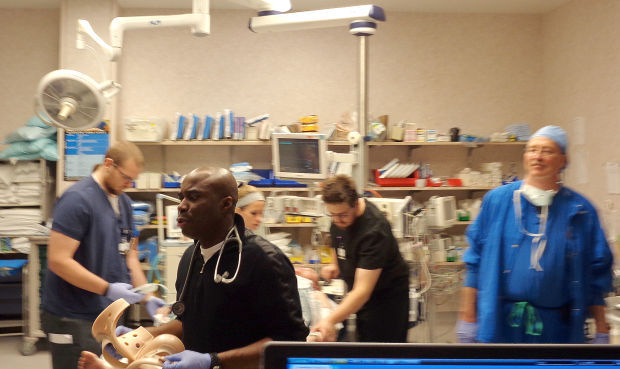
At Bryan West Campus, a Level 1 trauma center activation alerts roughly 30 people -- physicians, nurses, technicians, chaplains, registrars. Some set aside routines; others take up positions.
This image of people waiting, ready for patients to cross the threshold, is the quintessential trauma center picture, says Dr. Reginald Burton, medical director of what historically has been Nebraska's busiest trauma center.
People are also reading…
"It's the most organized chaos you'll ever see," he says.
A trauma center isn't a place anyone hopes to go, but those who need it wouldn't want to go anywhere else.
It's expensive care, with lots of highly trained people. But for those who crash, for kids nearly drowned, for drunks falling off walls, it can make the difference between full recovery and lifelong disability, or between disability and death.
They don't call them accidents here. They're crashes, falls. Accidents happen, Burton says. They're acts of God. Crashes and falls, however, are preventable. When a person gets drunk and falls from a roof, he says, "There was a high probability of that happening."
The other term trauma center workers bristle at is "local hospital," as when news anchors say the accident victim was taken to a "local hospital."
More precisely, they were taken to one of Nebraska's four primary trauma centers.
Let's break it down.
What is trauma?
Listen to that emergency dispatcher, and you'll hear her use the word to describe horrific crash injuries but also to describe a child's broken arm.
Trauma equals injury, Burton says. Injuries range in severity, but trauma center activation comes in three stages.
* Category 1: Life-threatening. Holes in the body from bullets or blades; brain visible; on the verge of coding -- imminent failure of the cardio-pulmonary system.
* Category 2: Linked to mechanisms of the injury: a person thrown from a car; falls of more than 10 feet.
* Category 3: Lesser injuries.
Trauma is easily explained, but a trauma center not so much. It's all of the following contradictions and more: a dozen full-time staff but also the resources of an entire hospital. A fraction of the hospital emergency room but also a statewide system reaching beyond walls into ambulances, rural hospitals, classrooms.
What it's not is a patient arriving at a hospital, waiting for an emergency room doctor to evaluate, waiting for blood to be ordered, waiting for a CT scanner to open, waiting for a surgeon and surgical suite. Because that adds up, Burton says.
"It's the right patient getting to the right place at the right time," Burton says, and it's a money quote regardless of who first coined it.
In 2002, Nebraska built a statewide trauma system around four Level 1 and Level 2 trauma centers in Lincoln, Omaha, Kearney and Scottsbluff. Very little differentiates Level 1s from 2s. Both are advanced.
Level 1 requires trauma research and residency programs. Bryan lacks the latter, the physician training component.
Along with advanced capabilities, levels 1 and 2 need surge capacity, says Bryan Trauma Program Manager Robbie Dumond.
"Most car crashes don't involve just one person," he says.
Adds Burton: "We've had up to five (patients) without declaring a disaster."
The Nebraska Medical Center and CHI Health Creighton University Medical Center in Omaha are the state's only Level 1 trauma centers. Previously, NMC and CUMC jointly shared the Level 1 designation.
Historically, Bryan's center, which sees 20 percent of roughly 8,000 annual trauma activations statewide, has been the busiest. Last year, its doors opened for 250 Category 1 patients, 800 Category 2s and 550 Category 3s. That doesn't count walk-ins like the guy with a gunshot wound dropped off by a buddy.
It's a lot, but compare that with the 33,952 emergency department visits to Bryan East Campus last year, the 35,865 to Bryan West Campus, the 6,237 visits to West for emergency mental health. Trauma activations account for just 2 percent of total emergency department visits.
Nebraska also has four Level 3 trauma centers, in Grand Island, Hastings, Columbus and North Platte. Surgeons stand available, but maybe they lack neurosurgeons.
Nebraska has numerous Level 4s, which range in size and ability. There's a different expectation, Burton says.
For serious injuries, "They can resuscitate and transfer to a higher-level center," he says.
Twenty-nine Level 4 hospitals typically send patients Bryan's way.
For more than five years, rural hospitals also have had the ability to consult with Bryan via two-way video. It's used mostly for clinical follow-ups -- checking on tracheostomy wounds, evaluating pain, screening for PTSD -- but it also helps prepare Bryan's team for what's coming. Sometimes, it's used for heart-wrenching cases, such as pediatric codes -- dying children.
Overall, Burton says, the idea of the statewide trauma system was that no matter where in Nebraska a person gets injured, he or she can get lifesaving care.
Bryan Trauma Outreach and Injury Prevention Coordinator Heather Talbot takes the trauma center concept beyond the hospital walls. She takes a trauma mannequin to rural hospitals so staff there can practice resuscitation and ensure they know where equipment is and whether it works. She speaks to schools about texting and driving, seatbelts, wearing bicycle helmets -- lessening injuries before they happen.
But to a mother and daughter recently pulled from twisted hot metal, what matters is the waiting team.
First responders communicate concerns, lighting up neurological pathways to care at the hospital. For the bleeding girl, five units of O negative blood stand ready inside a trauma bay, with quick access to gallons more -- a recent case required 40 units.
A pharmaceutical dispenser stands fully stocked in the bay, where the air temperature is a steady 80 degrees to help patients going into shock.
The team swarms as the doors open. An expansion and renovation in 2004 allows for back-hallway access to move bloodied patients to CT scanners, interventional radiology or to a room-sized elevator leading to intensive care.
In the doorway between two of the four main trauma bays, a lead physician, the captain of the ship, stands back and directs the two busy teams. Often, he appears to take everything in quietly as others scurry.
"If the captain has to tighten every rope," Burton says, "it's hard to tell where the ship is going."
Family begin arriving, and the chaplain deals with secondary trauma, the emotional blow. He keeps them informed.
One person in each bay collects data, adding to a database used for continuous improvement. Research occurs on the optimal use of blood fractions, on insulin, every little thing that keeps people alive.
That's how they're able to do the job, Burton says.
"People wonder how we can see such things and continue," he says.
Looking constantly to improve makes it possible.
Not every patient who arrives carries health insurance, and the money to maintain this system in continuous alert is a constant issue with lawmakers.
But better than 97 percent of those who arrive with signs of life survive.
Most will stay in a trauma bay no longer than 20 minutes before moving on to the next stage of care.
It's clockwork. Every second counts.
"We've been a trauma center since the '80s," Burton says. "This is not our first rodeo."